Delaying your dental visits due to COVID-19 can put you more at risk for gum disease and its complications. As dental practices implement stringent safety protocols and more Americans are getting vaccinated, it’s about time to let a dental professional evaluate your oral health.
You’ll never know the hidden attacks of bacteria in your mouth unless it starts to get painful or swollen. However, a sneaky disease like gum disease is a known silent killer. It can start from simple plaque to a full-blown irreversible dental condition that causes several health complications.
Health risks of gum disease
The chronic inflammation involved with gum disease or periodontitis increases the risk for tooth loss, systemic diseases, and stroke. The bacteria causing the gum disease can also enter the bloodstream, attack other parts of your body, and spread inflammation.
Gum disease has been linked to several medical conditions such as:
- Diabetes: The bacteria in gum disease triggers an immune response to fight the infection and cause an increase in blood sugar levels. Rather than be eliminated, the presence of sugar helps bacteria thrive and makes them multiply. Therefore, gum disease makes it hard to control the blood sugar levels of diabetic patients. At the same time, diabetes makes gum disease difficult to manage due to a weakened immune system.
- Rheumatoid arthritis: The immune response of the body to fight off gum disease causes a spike in protein levels in the body. The increased protein in the bloodstream can develop into rheumatoid arthritis or even make it difficult to manage.
- Alzheimer’s disease: Porphyromonas gingivalis is a bacteria found in both Alzheimer’s and gum disease patients. Gum disease patients are more at risk to develop Alzheimer’s since the bacteria can travel through the bloodstream and affect the brain.
- Pneumonia and Chronic obstructive pulmonary disease (COPD): The bacteria found in periodontitis causes a systemic inflammation that infects the lungs and the respiratory system. The inflamed airways and other symptoms of lung disease make it more difficult for patients to breathe and manage the disease.
Severe COVID-19 complications
Gum disease impairs your immune system’s ability to fight off other diseases and viral infections like COVID-19. According to the report from Wall Street Journal, periodontitis can cause severe complications to COVID-19 patients, such as increased ICU admission, need for oxygen assistance, and mortality rate.
The fatal impact of periodontitis on COVID-19 patients largely attributes to systemic inflammation and increased white blood cell levels.

The early warning signs and progression of gum disease
Periodontal gum disease begins with the bacteria between your teeth and gum line. With the presence of starch and sugar, the disease-causing bacteria create an environment or an invisible sticky biofilm around your teeth that turns into plaque.
The bacteria in plaque release acids that weaken your tooth enamel and cause cavities. On the other hand, they also irritate your gums and cause gum swelling, which is the early stage of periodontitis called gingivitis.
Gingivitis
Gingivitis is the inflammation of the gums around your tooth due to the formation of plaque or tartar. It is commonly caused by poor oral hygiene and few to no visits to a dentist or dental hygienist for a professional cleaning. Gingivitis is the treatable stage of periodontitis.
If left untreated, the bacteria will damage the gum tissues and bones that eventually leads to periodontitis. Visit your dentist as soon as possible if you experience any of the following:
- Swollen gums with unusual color like bright red or purple
- Gums that feel tender and bleed easily
- Pink bristles or the presence of blood when flossing and brushing your teeth
- Bad breath
- Abscess between your teeth and gum line
- Loose teeth or tooth loss
- Receding gums
- Painful gums when you bite
Lifelong treatment for gum disease
Once gingivitis has progressed to periodontitis, it becomes a point of no return and becomes irreversible. Periodontal treatments are only focused on managing the disease by removing plaque above and below the gum line to control inflammation and restore the structure of your teeth and gums. They include:
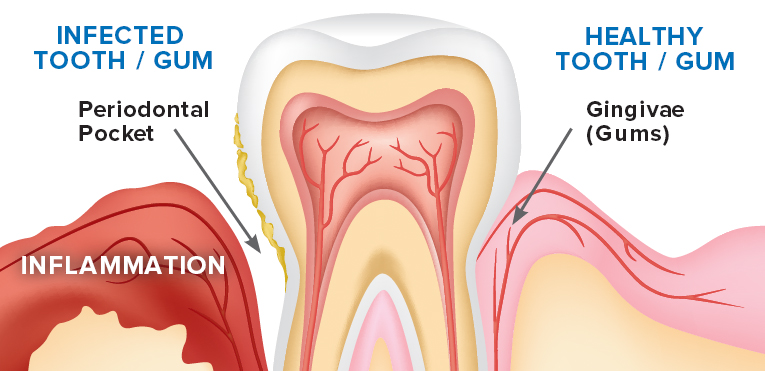
- Scaling and root planing: When the gums start to pull away from your teeth due to tissue damage, they create pockets. Scaling removes the plaque in the pockets below the gum line. Root planing smoothes the tooth root to encourage the gums to snuggle back the tooth.
- Bone and tissue grafting: In severe cases of periodontitis, the bone and tissue damage requires surgical treatments by grafting bone and gums. These treatments use a fragment of bone or a flap of gum to encourage the regeneration of your damaged bones and gums.
- Dental implants: To address tooth loss associated with gum disease, dentists recommend dental implants to restore the patient’s ability to eat and speak properly.
- Laser treatments: Like scaling and root planing, laser therapy removes the plaque and tartar above and below your gum line. It also smoothens the tooth to prevent bacteria build-up and removes the inflamed gums around the area.
Save yourself from the perils of gum disease by scheduling an appointment now
Prevention is the key to save yourself from the downhill impact of periodontitis on your health. Practice good oral hygiene by brushing your teeth twice a day. Flossing works wonders in preventing the formation of plaque between your teeth and gums.
Above all, visiting your dentist after several delays due to COVID-19 can help diagnose the early stage of periodontal disease and curb its progression as early as possible.
LandMark Dentistry provides dental cleanings and periodontal therapy in Charlotte, Wesley Chapel, Mallard Creek, and Matthews. Our team ensures your safety against COVID-19 by implementing stringent safety protocols. Check our safety guidelines here and schedule your appointment today.
